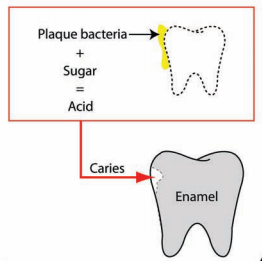
I’d like to keep my teeth healthy for as long as possible. I brush my teeth in the morning and at night, and floss every night, because daily flossing is associated with reduced mortality risk (https://atomic-temporary-71218033.wpcomstaging.com/2014/07/23/dental-floss-cancer-and-mortality-is-there-an-association/). Is there anything else that I can do to optimize my oral health? To answer that question, it’s important to know how tooth decay (also known as caries) occurs. As shown below, bacteria located on our teeth (in plaque) use dietary sugars to make acid, which demineralizes tooth enamel, thereby resulting in caries (Limeback et al. 2012).
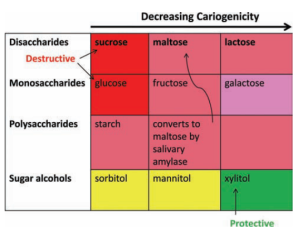
Not all dietary sugars are equal in their ability to produce tooth decay. In the picture below, sugars with red boxes are the most cariogenic. For example, the worst offenders in terms of tooth decay are sucrose and glucose. Also note that starch is cariogenic, but less when compared with sucrose and glucose. The least cariogenic sugars are sorbitol and mannitol, and, the sugar xylitol has been shown to be protective against tooth decay (Limeback et al. 2012).
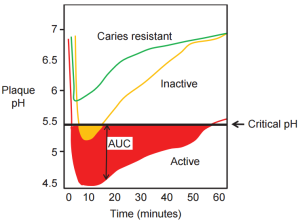
After eating a high sugar meal, there is an oral bacteria-induced increase in acidity that can lead to tooth demineralization. At an oral plaque pH of 5.5, tooth enamel demineralization occurs (Stephan and Miller 1943). Shown below is a graph of plaque pH vs. time for the 60 minutes following an oral glucose rinse. The green line is indicative of someone who is caries resistant: their plaque pH decreases from ~6.8 to ~5.8, followed by a relatively quick return to the starting pH value after 60 minutes. Note that at no point does the green line drop below the 5.5 threshold for enamel demineralization to occurr. The yellow line is indicative of someone at moderate tooth decay risk: their plaque pH drops from 6.8 to below 5.5, where it remains for ~ 10 minutes, and then slowly returns to baseline pH values after 60 minutes. The red line is indcative of someone that is at high risk for tooth decay: after the glucose rinse at time 0, their plaque pH rapidly drops below 5.5 and remains there for ~50 minutes, where significant teeth demineralization may occur. Note that their plaque pH doesn’t return to the baseline pH value after 60 minutes, either.
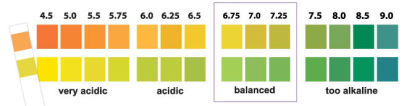
With these data in mind and my goal to reduce tooth decay risk I bought pH strips to test my daily oral pH. Shown below is what the pH strip looks like, without having been dipped in my saliva. Adjacent to that is the pH color scale, and to the right, my average daily fasted oral pH, ~6.5:
The good news is that I’ve yet to see an oral pH value below 6.5, which puts me at low risk for tooth decay. To further minimize that risk, in addition to brushing and flossing, after meals and throughout the day I gargle with a homemade 1% sodium bicarbonate (physiological saline is ~0.9%) and 10% xylitol solution. I use sodium bicarbonate to temporarily neutralize any potential oral acids. Xylitol can protect against tooth decay by reducing plaque and the level of tooth decay-causing bacteria (i.e. Streptococci mutans) in saliva and plaque (Söderling 2009). For example, fluoride-containing toothpaste in the presence of 10% xylitol reduces tooth decay more than fluoride toothpaste alone (Sintes et al. 1995; Sintes et al. 2002). However, it’s important to note that some xylitol-based studies have not been shown to reduce tooth decay risk (Riley et al. 2015). At worst, including xylitol may have no effect, whereas at best it may reduce oral Streptococci mutans, thereby decreasing tooth decay risk.
After gargling, my normal oral ph (~6.5) changes to alkaline (~8.5), as shown in the pH strip below:
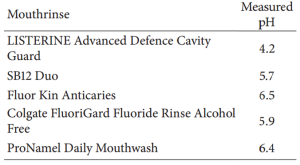
Couldn’t I use a store-bought mouthwash instead? The measured pH of several commercially available mouthwashes is shown in the table below (Sun et al. 2014). Note that some are below the critical pH for tooth demineralization, 5.5! Others aren’t too far away from 5.5, either. In contrast, the pH of my homemade mouthwash pH is ~8.0.
If you’re interested, please have a look at my book!
References
Limeback H et al. Comprehensive Preventive Dentistry, Chapter 1: “A brief introduction to oral diseases: caries, periodontal disease, and oral cancer”. page 1-24. July 2012. ISBN: 978-0-8138-2168-9.
Riley P, Moore D, Ahmed F, Sharif MO, Worthington HV. Xylitol-containing products for preventing dental caries in children and adults. Cochrane Database Syst Rev. 2015 Mar 26;3:CD010743.
Sintes JL, Escalante C, Stewart B, McCool JJ, Garcia L, Volpe AR, Triol C. (1995). Enhanced anticaries efficacy of a 0.243% sodium fluoride/10% xylitol/silica dentifrice: 3-year clinical results. American Journal of Dentistry, 8, 231–235.
Sintes JL, Elías-Boneta A, Stewart B, Volpe AR, Lovett J. (2002). Anticaries efficacy of a sodium monofluorophosphate dentifrice containing xylitol in a dicalcium phosphate dihydrate base. A 30-month caries clinical study in Costa Rica. American Journal of Dentistry, 15, 215–219.
Söderling EM. (2009) Xylitol, mutans streptococci, and dental plaque. Advances in Dental Research, 21, 74–78.
Stephan RM and Miller BF. (1943) A Quantitative Method for Evaluating Physical and Chemical Agents which Modify Production of Acid in Bacterial Plaques on Human Teeth. Journal of Dental Research, 22, 45–51.
Sun FC, Engelman EE, McGuire JA, Kosmoski G, Carratello L, Ricci-Nittel D, Zhang JZ, Schemehorn BR, Gambogi RJ. Impact of an anticaries mouthrinse on in vitro remineralization and microbial control. Int J Dent. 2014;2014:982071.




http://www.ncbi.nlm.nih.gov/pubmed/24852946
LikeLike
I have data in submission that links circulating erythritol with increased inflammation. So I’ll pass on an erythritol rinse…Nonetheless, good
post!
LikeLike
I would love to see such data that shows a truly significant increase in systemic inflammation (especially if you are restricting its use to gum or a rinse) over Xylitol. I look forward to your post with references. Granted there is far less data on Erythritol compared to Xylitol, but in any study I’ve read thus far that includes both, Erythritol beats out or equals Xylitol for its stated/given use. I use very little of either (or any sweetener) but Erythritol has replaced Xylitol in some of my teas that would be a tad bitter sans any sweetener. For a rinse it is fine, but as a sweetener I find it intolerable.
LikeLike
You´re focussing on ph-level of the mouthwash, but the mouthwash targets the bacteria / plaque which is the cause of the acid and not the acid itself. So while a high acid / low ph mouthwash might (intuitively I would agree, but I´ll look into it) be a bad idea, it´s function is not primarily antacid, but disinfecting (among others regarding mouth flora).
LikeLike
That doesn’t make sense-acid is the stimulus for tooth demineralization. If the mouthwash is acidic, it will contribute to that process.
LikeLike
Sorry, that is not what I meant. I meant basic / low ph mouthwash, which is why in the last sentence I wrote about it antacid function.
LikeLike
This site has some interesting ideas along these same lines, relative to pH of mouthcare products, timing of toothbrushing, xylitol, etc. I’ve linked to one, but you can find others in amongst the comments and his orthodontics articles. All of this makes sense, but I wonder why I get quizzical looks when I mention such at my dental visits?
http://www.freysmiles.com/blog/view/should-you-brush-teeth-before-or-after-eating
LikeLike
Why rinse? Why not add nitrite rich vegetables to your diet?
Our salivary glands actively accumulate nitrate from the blood and secrete it with the saliva into the mouth. The bacteria that can breath NO3 (denitrifying bacteria) will use it and produce NO2. These bacteria do not produce acid, but when close to an acid producing bacteria the nitrite will react with the acid and kill the acid producing bacteria.
And by eating nitrite you can kill potential pathogens in the stomach through the nitrite-stomach acid reaction.
See bottom for a list of relevant studies: http://www.berkeleytest.at/kariesschutz/
LikeLiked by 1 person
This is THE most informative comment on dental health that I have read to date, I will tell you from experience that if I drink a juice that contains 8 oz of fresh beets my saliva PH will rise significantly in a few hours. After reading some of the studies you linked to I now know why,
This is a grossly overlooked factor in dental health, I am going to try other nitrate sources to see if I get the same effect, Radishes, butterhead lettuce, cilantro even the Chinese herb danshen are supposed to be good sources. Thanks for the links! Lots of food for thought and health!
LikeLike
As you can see on my blog, I do indeed eat lots of nitrite-rich vegetables, including beets and green veggies. Have you done the experiment on yourself to make sure your oral pH doesn’t drop below 5.5?
LikeLike
I know you do, and because your PH never dips really low, I guess the rinsing is overkill, but you need something to blog about 🙂
I never have had caries or dental problems, but I have not tested myself. That will be a fun thing to do this weekend with the swimming pool kit. I do avoid sour fruits though.
LikeLike
I tested myself many times-fasted, immediately after eating, 1-2-4-8 hours after eating, etc. Yes, I’m fortunate about that now, but my diet was not great for 40ish years, and I probably rotted my teeth more than I should have without a proper diet and optimal oral hygiene.
LikeLike
From the nitrites point of view, does it matter if you eat the beetroot raw or cooked?
LikeLike
To answer that question, you’d have to look up the data on whether there are cooking-induced loss of nitrates. That I don’t know off the top of my head, but to be safe, almost every day I have spinach or beets (at the very least) in my diet, to make sure I get a good amount of nitrates.
LikeLike
What is the best period after eat to brush your teeth? I heard that brush just after the meal could improve demineralization due to the acid saliva. Is that true?
LikeLike
That is true. To minimize that, I gargle/rinse with my bicarbonate-xylitol homemade mouthwash. Then, I floss, followed by brushing, and I gargle with that mouthwash again. The mouthwash is alkaline (ph ~8), so garglinging/rinsing with it prior to brushing should minimize any acidity in my mouth.
LikeLike
What is the best technique to brush your teeth? Bass, Modified Bass, Stillman, Toothpick method (Watanabe), etc.
LikeLike
As long as they get brushed, I don’t think the technique matters. But maybe there’s published evidence to dispute that idea?
LikeLike
I don’t know, maybe it matters after all.
https://www.researchgate.net/publication/7321779_Comparison_of_modified_Bass_technique_with_normal_toothbrushing_practices_for_efficacy_in_supragingival_plaque_removal
http://www.ncbi.nlm.nih.gov/pubmed/9797056
LikeLiked by 1 person
Here’s a video on how to perform the modified Bass technique:
LikeLike
Hi Michael, i’m currently researching the exact same topic. I think you should investigate further about “plaque ph”. This is the real cause for caries. It even can be measured easily. You can use normal ph strips (eg. Merck). They can be cut in 2mm stripes. You should not brush your teeth one day. Afterwards the plaque ph level can be measured between the teeth by holding 10 sec. It should not be less than 5.5.
LikeLike
Do you subscribe to the idea that certain volatile oils such as peppermint oil can help fight gingivitis? If so, how much peppermint oil should be added to a glass of water for the desired effect?
LikeLike
Hey Zoltan, yes, there is data that peppermint oil may be beneficial for oral health-some of that data is in my book!
LikeLike
I just read your book – so would you add peppermint oil and flawseed oil to your mixture nowadays?
LikeLike
I add a drop or 2 of peppermint oil (and sometimes others like clove or cinnamon oil) on top of my toothpaste when I brush my teeth, and without quantifying the effect of it on my oral microbiome, it feels refreshing.
I regularly (~5x/week) consume ground flaxseeds every morning (~45g/day). I try to limit my oil intake, as it’s calorie dense but nutrient poor.
btw if you liked the book, please don’t hesitate to review it on Amazon! That always helps in spreading the word…
LikeLike