In an earlier post I wrote about the association between elevated circulating levels of homocysteine with an increased risk of death from all causes (https://michaellustgarten.wordpress.com/2017/11/22/homocysteine-and-all-cause-mortality-risk/). I started to post updates in that link, but I’ve decided to move them to here.
As of 6/2018, I now have tracked dietary data (I weigh all my food and record the values in cronometer.com) that corresponds to 7 homocysteine measurements:
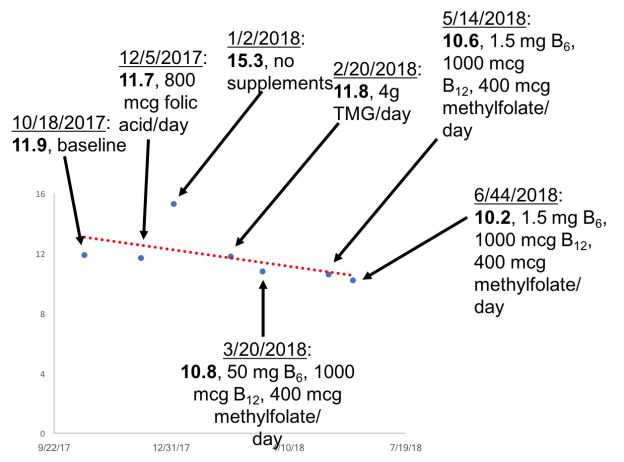
12/5/2017: Despite 42 days of 800 micrograms of supplemental folic acid, bringing my average daily folate intake to 2026 micrograms/day, my plasma homocysteine was essentially unchanged at 11.7 uMoL, when compared with my baseline value of 11.8 uMol.What’s next on the list to reduce it? Trimethylglycine, also known as betaine. I’m a proponent of using diet as a first strategy, and to increase my dietary betaine levels, I’ll eat beets and quinoa, bringing my daily betaine levels to ~500 mg/day. Let’s see how it turns out on my next blood test!
1/2/2018: ~500 mg/day of betaine from beets and quinoa did absolutely nothing to my homecysteine levels. In fact, it got worse (15.3 uMoL)! To test the hypothesis that it wasn’t enough betaine, next I tried 4 grams/day of betaine (also known as trimethylglycine, TMG).
2/20/18: Supplemental TMG did absolutely nothing in terms of reducing my homocysteine to values below baseline! Also note that there is evidence that TMG increases blood lipids, including LDL and triglycerides (TG; Olthof et al. 2005), and that’s exactly what it did to me. My average LDL and TG values since 2015 (11 measurements) are 77 and 50 mg/dL, respectively. On TMG, these values increased to 92 and 72 mg/dL, respectively, making them my highest values over 11 individual blood tests (with the exception of 1 day with an LDL of 93 mg/dL). Next, I tried a stack that included 50 mg of B6, 1000 mcg of B12, and 400 mcg of methylfolate, as supplementation with these B-vitamins has been shown to lower homocystine (Lewerin et al. 2003).
3/20/18: Finally, some progress! My homocysteine levels were reduced during the B-vitamin supplementation period. I’ve written it like that because I’m not sure if it was the B-vitamins that caused it. For example, in the image below, we see the correlation between my dietary B6 intake with homocysteine. The trendline is down, which I would expect if B6 supplementation actually is playing a role in reducing my homocysteine levels. However, note that the correlation between my dietary B6 levels with homocysteine is not very strong (r = .48), resulting in a moderate R2 of 0.23 (similar data was obtained for B12 and folate). With 5 blood test measurements corresponding to 5 dietary periods, if B6 is playing a role, I would expect a stronger correlation. Nonetheless, with more data, the correlation may strengthen, so stay tuned for that!

5/14/2018: I changed B6-B12-methylfolate supplements so that I’d only have to take pills from 1 bottle instead of from 3. That supplement, however, had 1.5 mg of B6 instead of the 50 mg that was in my original supplement. Less B6 didn’t result in a higher homocysteine value-in fact, it went down (slightly), from 10.8 to 10.6. If an increased amount of B6 was causing lower levels of homocysteine, I would’ve expected higher, not (barely) lower homocysteine levels. This suggests that maybe my B6 intake has nothing to do with my homocysteine levels.
6/4/2018: Despite no changes to my supplements, my homocysteine came down a little more, to 10.2. Interestingly, the correlation (r) between homocysteine with my total dietary (diet + supplements) intake of B6, B12, and methylfolate is 0.39, 0.68, 0.29, respectively. The correlation between my B12 intake with homocysteine looks moderately strong, whereas the correlations for B6 and folate are weak. Based on this data, it’s possible I had a mild B12 deficiency that was causing elevated homocysteine. Note that my average B12 intake, without supplements is ~8 mcg/day, which is more than 3-fold higher than the RDA.
In looking at the association between my dietary data with homocysteine, a stronger correlation (r = 0.91; R2 = 0.83) has emerged…for my protein intake! In other words, a higher protein intake is more strongly correlated with lower homocysteine than B12:
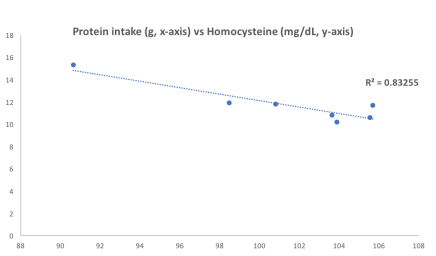
7/11/2018: To explore the strong association between my protein intake with homocysteine, I increased my protein intake from an average value of 104 g/day for the period that preceded my June measurement (5/15/2018 – 6/4/2018) to 136 g/day for the period up to my 7/11/2018 measurement (6/5/2018 – 7/10/2018). The result? Lower homocysteine, to 8.2 uMol/L! Interestingly, the correlation between my dietary protein intake with homocysteine remained strong (r = 0.86, R2 = 0.73, n = 7 measurements).
What about my B6, methyl-B12, methyl-folate stack? I’m still taking it, although it looks like methyl-B12 may be the only factor that is associated with my homocysteine levels. In support of that, the correlation between each with homocysteine is r = 0.02, 0.73, 0.36, respectively.
Because I now have my homocysteine < 9 umol/L, it may be time to optimize other variables (in addition to the metabolic panel and CBC). Stay tuned!
If you’re interested, please have a look at my book:
References
Lewerin C, Nilsson-Ehle H, Matousek M, Lindstedt G, Steen B. Reduction of plasma homocysteine and serum methylmalonate concentrations in apparently healthy elderly subjects after treatment with folic acid, vitamin B12 and vitamin B6: a randomised trial.vEur J Clin Nutr. 2003 Nov;57(11):1426-36.
Olthof MR, van Vliet T, Verhoef P, Zock PL, Katan MB. Effect of homocysteine-lowering nutrients on blood lipids: results from four randomised, placebo-controlled studies in healthy humans. PLoS Med. 2005 May;2(5):e135.

Michael have you found studies that show
Artificially lowering homocysteine extends lifespan and are not just caused by correlation between death and natural homocysteine levels?
LikeLike
There are indeed studies where homocysteine lowering doesn’t improve health-related outcomes. However, it’s associated or plays a causative role in lots of adverse-health related stuff, so I think it’s wise to nonetheless reduce it.
LikeLike
Wacky theory, but I wonder if the increased protein intake is letting you synthesize more creatine? And the increased creatine is lowering the homocysteine?
https://www.ncbi.nlm.nih.gov/pubmed/19079843
https://www.ncbi.nlm.nih.gov/pubmed/15168891
LikeLike
Could be, Dan. That’s a good hypothesis!
LikeLike
Hi, I know this is a little old this piece but is there an update? I can see that on your last reading you got levels to around 10 and was wondering if you had any more data? I know the standard Homocysteine reducing technique seems to revolve around folate but is supplementing folate that simple?
LikeLike
Hi Larson, my last reading was 7.3, on a blood test done Feb 12, 2019. I don’t think it’s a folate issue, as my diet provides 3x the RDA (1200 mcg/day), and taking a methylfolate (400 mcg)-methylB12-B6 vitamin didn’t reduce it much, maybe ~10%. Since I’ve upped my protein intake to 130-140g/day (from 100g/day), my homocysteine has consistently been lower than when I started (between 11-15).
LikeLike
Thanks Michael, that is really interesting. I recently increased my protein and reduced my vegetables and some of my markers got better. Noticeably my zinc went into range for the first time in 5 years. Eating less plants seems to have improved my digestion a lot too. All that said my Homocysteine went up a fair bit. So, as you have said on some of your videos, changing what you eat, potentially, have some benefits and some negatives, you just need to find out where your own N=1 range is. Onwards and upwards with you and your journey.
LikeLike
A good way to evaluate diet changes is by using aging.ai, which uses circulating biomarker data to construct a biological age. I have a post on that, too:
LikeLike
The basic level of analytes for aging.ai are on the CBC, which is a ~$35 test (I get it from lef.org). I’m not sponsored by them, but that’s what I use:
https://www.lifeextension.com/Vitamins-Supplements/itemLC381822/Chemistry-Panel-Complete-Blood-Count-CBC-Blood-Test
LikeLike
Noted, thanks.
LikeLike
Sorry to trouble you again Michael, but do you do your homocysteine checks fasted? I have read both fasted is good and also three hours after a protein meal is best? see: https://www.biolab.co.uk/print.php/cmsid__biolab_test/Homocysteine_-_plasma
LikeLike
Yes, fasted.
LikeLike
That’s awesome! I haven’t heard of aging.ai and I don’t quite have all the numbers to populate it but based on a variety of inputs, some omitted, I am both younger and older and both male and female so that is interesting! I will certainly give this platform some scrutiny for future data collection. And I might order a couple of nice dresses incase.
LikeLike
Pingback: Blood Urea Nitrogen: A Simple Blood Test For Determining Optimal Protein Intake – Michael Lustgarten
Does B12, B6, Folate increase the chances of cancer?
LikeLike
Why do you think that?
LikeLike
Have you looked into supplementing with NAC? It has also been shown to lower homocysteine, as well as raise glutathione (beneficial for immune system). It is also thought to reduce viral replication (think covid). https://www.italjmed.org/index.php/ijm/article/view/itjm.2019.1192
LikeLike
Thanks john1202, I may try NAC at some point!
LikeLike
I forgot to mention that intermittent fasting (eg. Ramadan dry fasting) has also been shown to lower H.
LikeLike
Yep, I already integrate IF into my my approach-for ex., yesterday I stopped eating at 2PM, and didn’t eat until 530 AM, so a 17.5 hr fast overnight.
LikeLike
Wow, 15.3 to 7.3…sounds like whatever you did to decrease your homocysteine, you definitely nailed it. The number of people who could benefit from this information is huge. And it was also fun to read the saga of your inputs and results, and try to test-drive my limited understanding of “one-carbon metabolism” as you went along. I have 2 questions:
1. Do you have any record of your serum B-12 status during this time? Though your diet supplies plenty (and not only B-12 but also methyl donors and co-factor B-6), I gather it is common amongst hypothyroid/Hashimoto’s pts to not absorb B-12 very well, and also to do better when they are at the high end of the range…closer to 700pg/mL. I would speculate that your higher Hcy results corresponded to a lower B-12 status, which your supplementation slowly corrected. Does this sound reasonable to you? Is your B-12 now high-normal?
2. I admit I don’t understand how consuming more “protein” would lower homocysteine. But the term “protein” obscures the variety of specific amino acids whose identity may become significant at the level of specific metabolic processes. I don’t suppose your nutrition software allows you to have any insight as to which amino acids (especially sulfur-containing methionine or cysteine) may have been disproportionately high or low during any given period. If you were vegetarian during any of this time, one might guess a shortage of these particular amino acids could limit either the trans-sulfuration to homocysteine and/or the methylation of homocysteine to (eventually) glutathione. Now that your homocysteine is down I would speculate that your CRP will also be lower, reflecting (all other things being equal) proper trans-sulfuration of methionine and methylation of homocysteine to glutathione.
LikeLike
I didn’t directly measure B12 in blood, but adding a methylfolate-methylB12-b6 supplement reduced my Hcy by ~10% before I increased my protein intake by an average of 30g/day, which also had an effect on reducing it. I wouldn’t say that B12 slowly corrected my Hcy, as it was ~3 consecutive months of ~10% reduced Hcy with it included, before I tried other interventions.
Cronometer tracks AAs, but not for all foods, so I’m not sure which AAs impacted Hcy. I don’t see a correlation for Hcy with CRP, for ex., when Hcy was high, CRP never went past 1 mg/L.
LikeLike
This article is most useful I’ve ever seen on Homocysteine ! Thanks so much for the excellent info 🙂
Does it make a difference what kind protein is used? Can strictly plant based protein drop the Hcy levels?
In the beginning of the article you state that you tracked 7 homocysteine measurements on cronometer, but I only saw a couple mentioned throughout the article : TMG, B6, B12 and folic acid (methylfolate). What were the other ones or I am missing something?
LikeLike
Thanks Jae. I’m not sure if it’s the type of protein, but for whatever reason a higher protein intake is correlated with lower homocysteine in my data. I now have 11 measurements, and the correlation for these 2 is still strong, r=-0.87, p=0.0005.
What I meant by the 7 measurements is that I have 7 dietary periods that correspond to 7 homocysteine blood tests. In the past I tried high dose TMG, and still take a methylfolate (400mcg), methyl B12 (1000mcg) and B6 (1.5mg) supplement. I may get rid of that, though, to see if it’s actually doing anything in terms of homocysteine.
LikeLike
N aceylcysteine (NAC) has also been shown to lower homocysteine (and blood pressure). I have found that NAC with vitamin C lowers my refractory BP within a couple of hours – much better than pharma medication.
LikeLike
Thanks Michael! Ok got it.
Likewise, I have a preference for resolving issues using dietary means so I’m keen to see what a increase in protein does for me. Keep up the great work:)
LikeLike