After going on Joe Rogan’s podcast, Paul Saladino, MD, posted his show notes, which included his blood test results. Based on that data, is his biological age optimal while on a carnivore diet?


After going on Joe Rogan’s podcast, Paul Saladino, MD, posted his show notes, which included his blood test results. Based on that data, is his biological age optimal while on a carnivore diet?

Here’s a podcast that was recorded with WildHealth, enjoy!

The incidence of fungi bloodstream infections increases during aging-is that a potential explanation for the presence of fungi in the brains of Alzheimer’s disease patients? Rapamycin is a known antifungal-is it effective against fungi that are found in the blood and brain?
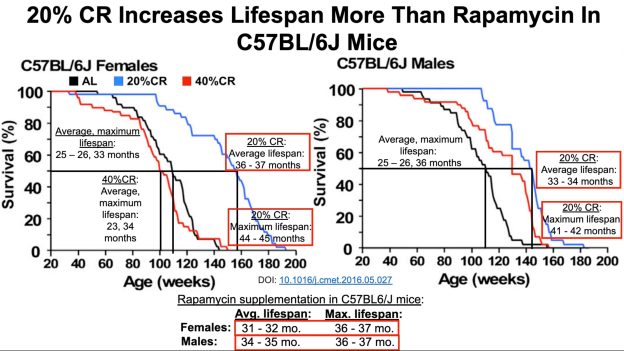
Maximal lifespan in calorie restricted (CR) mice can range from 45 – 55 months. In this video, I present data for 3 studies on rapamycin-can it beat CR for maximal lifespan?

LPS increases during aging, which may explain the age-related increase for CD38 and decreased NAD+. LPS is decreased on a calorie restricted diet, but what else can reduce it? In this video, I present evidence for intestinal alkaline phosphatase’s (IAP) role on LPS, and posit that interventions that increase IAP may be an important approach for increasing NAD+.

My latest blood test results are in-how’s my biological age? In the video I discuss my dietary approach prior to my latest blood test, the blood test results, and my plan to improve them going forward.
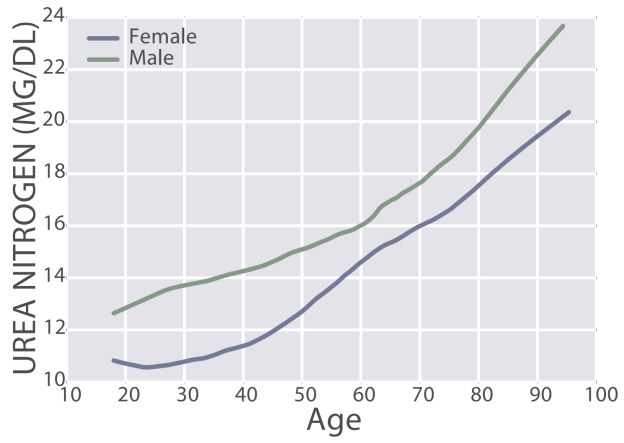
Blood urea nitrogen (BUN) is one of the 19 variables found on the biological age calculator, aging.ai. It measures the amount of nitrogen, as contained in urea (i.e., blood urea nitrogen, BUN) in your blood. The reference range for BUN is 5 – 20 mg/dL, but within that range, what’s optimal?
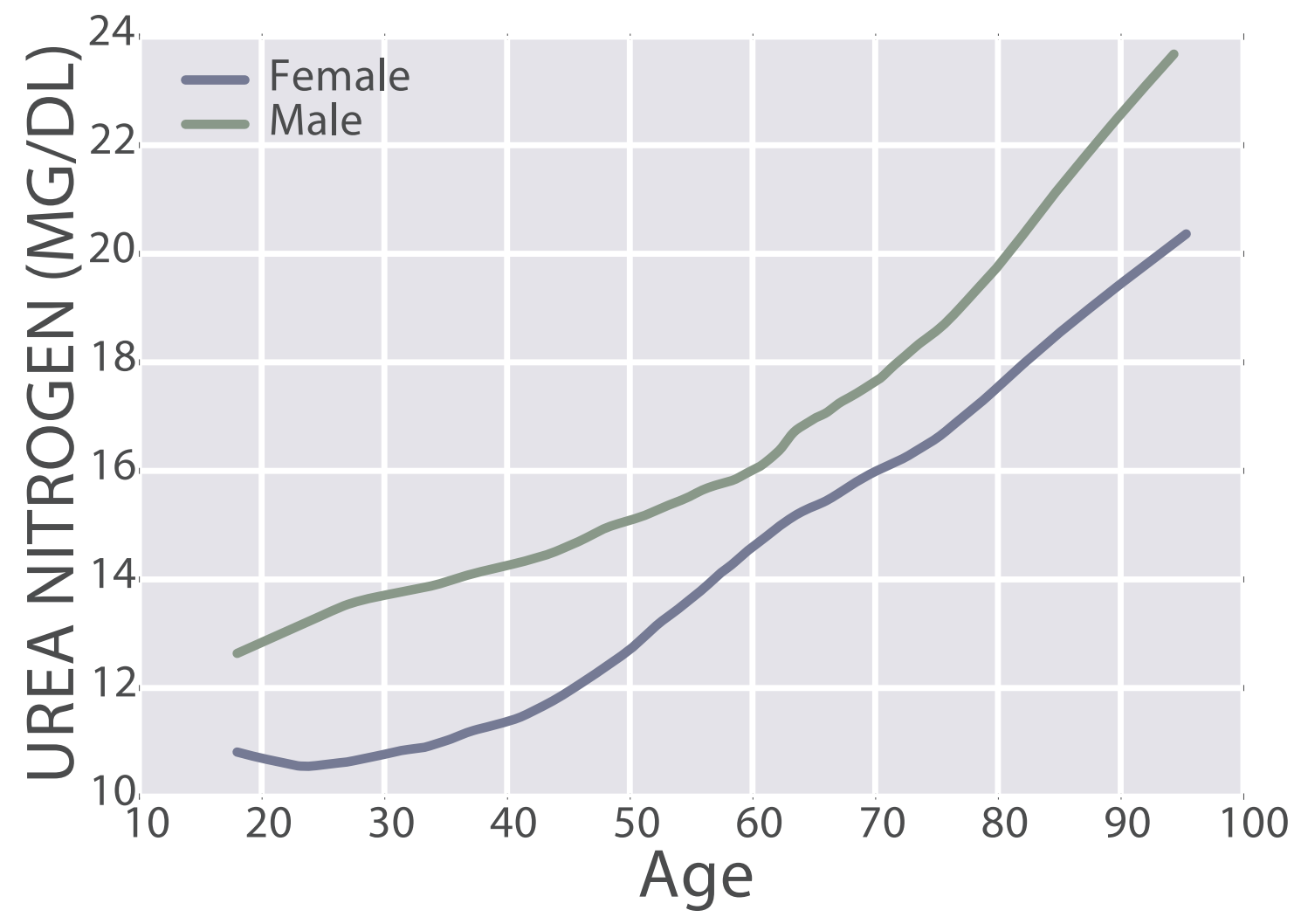
First, BUN increases during aging, from 11 – 13 mg/dL in 20 yr olds to 20 – 22 mg/dL in 90 yr olds (Wang et al. 2017):
The importance of the age-related increase in BUN is illustrated by the finding that risk of death for all causes increases above 15 mg/dL:

Also note that maximally decreased risk for all cause mortality was associated with BUN values between 5 – 15 mg/dL. In addition, even though a BUN value = 20 mg/dL is technically within the reference range, risk of death for all causes would be 50% higher when compared with someone that had BUN levels between 5 – 15 mg/dL. Collectively, based on the aging and all-cause mortality data, I’d argue that 5 – 13 mg/dL may be the optimal range for BUN.
Assuming normal kidney function (see https://michaellustgarten.wordpress.com/2019/11/18/optimizing-biologic-age-creatinine/), if your BUN is higher than 15 mg/dL, can it be reduced? Note that urea production is almost perfectly correlated (r = 0.98) with dietary protein intake (Young et al. 2000):
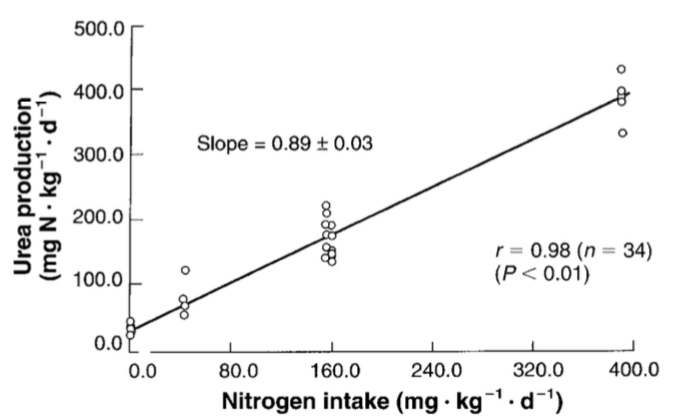
In other words, the main source of dietary nitrogen is protein, so if you eat a lot of protein, you’ll make a lot of urea. Circulating levels of urea can be easily calculated by measuring BUN, via: Urea [mg/dL]= BUN [mg/dL] * 2.14). Therefore, measuring BUN can then be used to determine if your protein intake is too high or too low.
What’s my BUN? As shown below, I’ve measured BUN 22 times since 2015. In line with the Young et al. (2000) data that showed an almost perfectly linear correlation between dietary nitrogen intake with urea production, similarly, as my dietary protein intake has increased, so have my BUN levels. The correlation between my dietary protein intake with BUN is strong (r = 0.76, R^2 = 0.575, p-value = 4.3E-05):
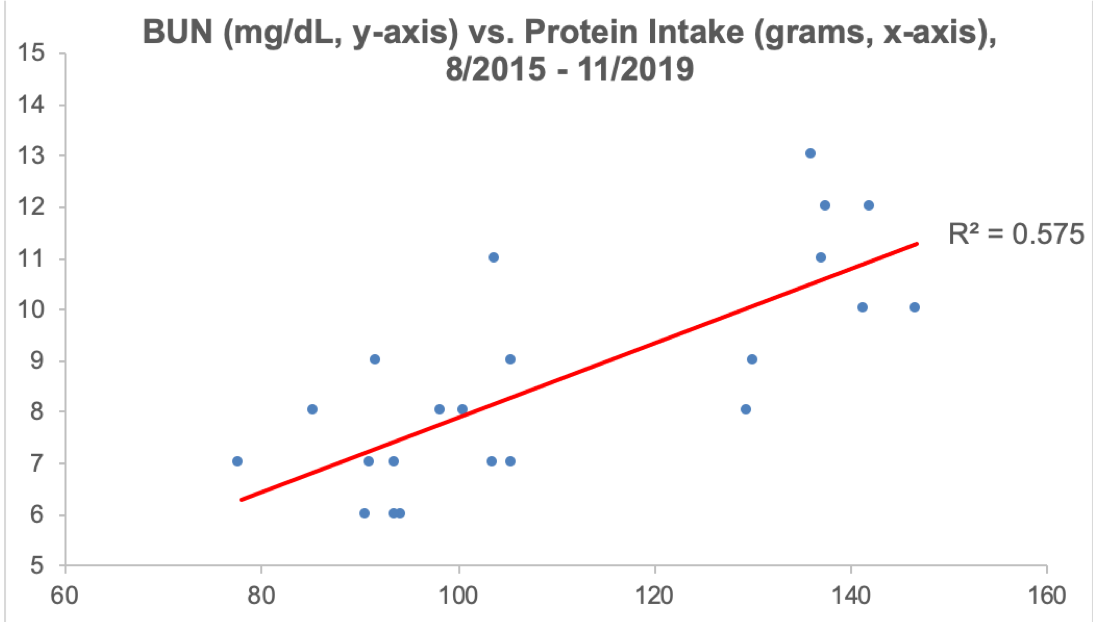
Note that my BUN is (purposefully) below 15 mg/dL, the upper limit for reduced all-cause mortality risk in Solinger and Rothman (2013), and within the 11 – 13 mg/dL range reported for the 20 yr olds of Wang et al. (2017).
For more recent tracked data, see the video!
References
Solinger AB, Rothman SI. Risks of mortality associated with common laboratory tests: a novel, simple and meaningful way to set decision limits from data available in the Electronic Medical Record. Clin Chem Lab Med. 2013 Sep;51(9):1803-13.
Wang Z, Li L, Glicksberg BS, Israel A, Dudley JT, Ma’ayan A. Predicting age by mining electronic medical records with deep learning characterizes differences between chronological and physiological age. J Biomed Inform. 2017 Dec;76:59-68. doi: 10.1016/j.jbi.2017.11.003.
Young VR, El-Khoury AE, Raguso CA, Forslund AH, Hambraeus L. Rates of urea production and hydrolysis and leucine oxidation change linearly over widely varying protein intakes in healthy adults. J Nutr. 2000 Apr;130(4):761-6.
If you’re interested, please have a look at my book!


Although many of my posts aimed at improving health and longevity are focused on diet, in this post I’ll show data that demonstrates that I’ve been able to steadily improve my cardiovascualr fitness. In earlier posts I reported that a resting heart rate (RHR) of 40 beats per minute (bpm) was associated with lowest risk for all-cause mortality (https://michaellustgarten.wordpress.com/2019/02/02/resting-heart-rate-whats-optimal/), and I noted my own RHR progress in a year-over-year update, from values of 51.5 – 52.7 bpm in August – Sept 2018 to 49.3 – 48.7 bpm during the same months in 2019 (see https://michaellustgarten.wordpress.com/2019/10/08/resting-heart-rate-year-over-year-update/). Have I continued to make progress?
Shown below are 2 more months of RHR data, from August – November 2018, and the data for those months in 2019:
 From August – November 2018, I reduced my RHR from ~52 to 50 bpm, whereas in 2019, I made smaller progress, but the trend is still downward, from 49 to 48 bpm. The 2018 data is significantly different from the 2019 data, as assessed by single-factor ANOVA (p = 8E-14).
From August – November 2018, I reduced my RHR from ~52 to 50 bpm, whereas in 2019, I made smaller progress, but the trend is still downward, from 49 to 48 bpm. The 2018 data is significantly different from the 2019 data, as assessed by single-factor ANOVA (p = 8E-14).
Adding strength to these findings is that my heart rate variability (HRV), as a second index of cardiovascular health, has increased during the same period:
 Note that from August – November 2018, my average daily HRV value never topped 48, whereas during the same 4 months in 2019, it was never lower than 52.1, with my best ever HRV values found in November. The 2018 is significantly different when compared with 2019, again based on single-factor ANOVA (p = 5.2E-13).
Note that from August – November 2018, my average daily HRV value never topped 48, whereas during the same 4 months in 2019, it was never lower than 52.1, with my best ever HRV values found in November. The 2018 is significantly different when compared with 2019, again based on single-factor ANOVA (p = 5.2E-13).
How am I improving my cardiovascular fitness? That’s a topic for another post, but note that my strength is still pretty good, as evidenced by my 12 pull-ups in the video below!
https://www.youtube.com/watch?v=dLktQvFz70Q
If you’re interested, have a look at my book!
The percentage of lymphocytes is one of the 9 blood test variables included in the biological age calculator, Phenotypic Age (https://michaellustgarten.wordpress.com/2019/09/09/quantifying-biological-age/). The reference range for lymphocyte % is 20 – 40% of the total amount of white blood cells (WBCs), but are higher or lower values optimal for health and longevity?
To answer that question, it’s important to know how levels of lymphocytes change during aging, and its association with risk of death for all causes. In one of the earliest studies to examine how the percentage of lymphocytes changes with age, Levine (2013) reported that lymphocyte % significantly decreased during aging in 9,389 adults (age range, 30 – 75y). However, the absolute values for these changes, i.e. from 40% to 30%, for ex., was not reported.
Similarly, lymphocyte % decreased during aging in a much larger study (377,686 subjects; age range, 18 – 85y; Wang et al. 2017):
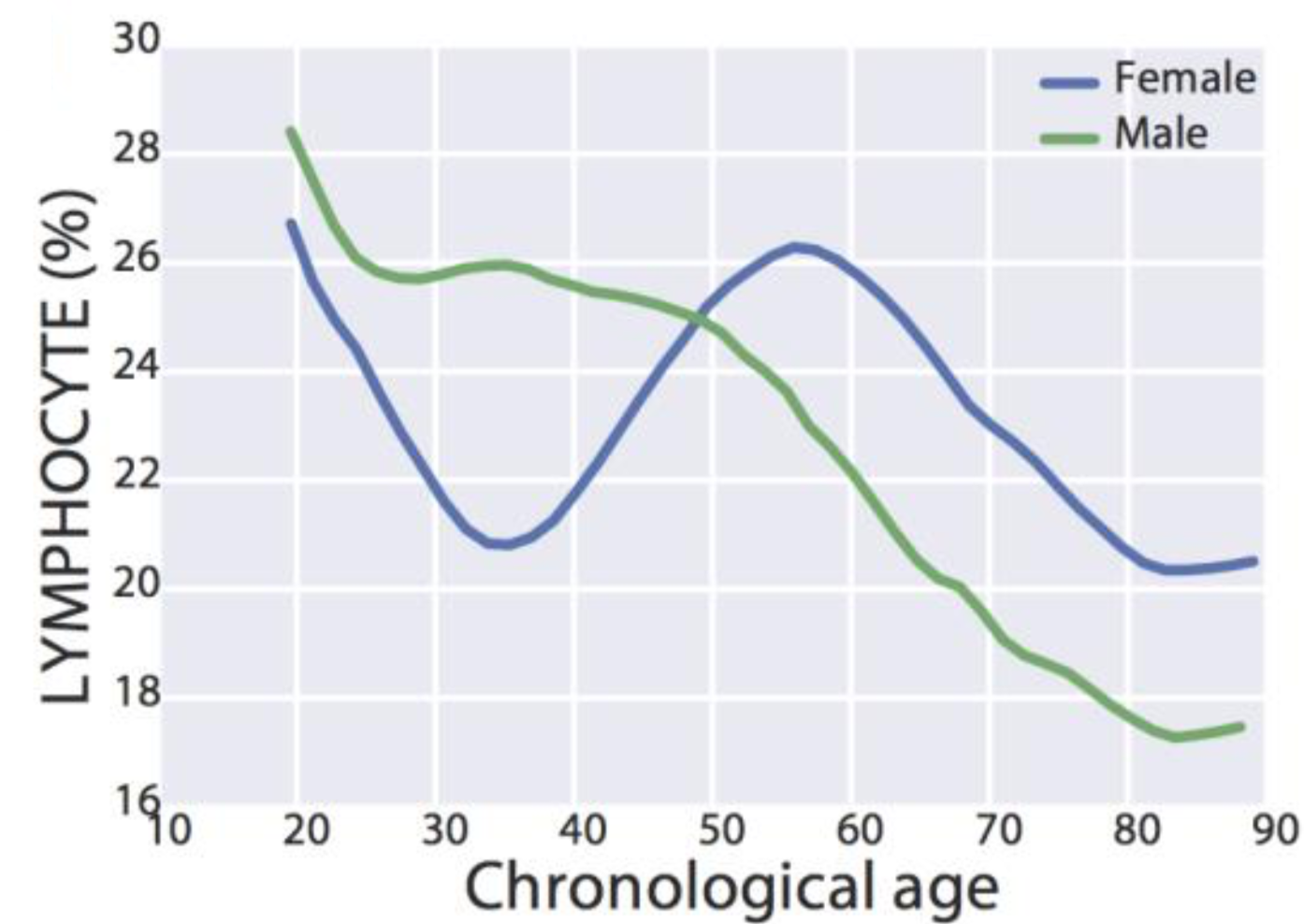
Interestingly, for women, lymphocyte % decreased from 27% to 21% from 20 – 35y, increased from 21% to 26% from 35 – 55y, then again decreased from 26% to 20% from 55y to 85y. In contrast, lymphocyte % more steadily decreased for men, from 28% to 17% from 20 – 85y.
Based on the aging data, higher values for lymphocyte % are are associated with biologic youth, whereas lower values are found in older adults. Although there are few studies that have investigated associations between lymphocyte % with aging or disease risk, in contrast, more studies have been published for absolute levels of lymphocytes.
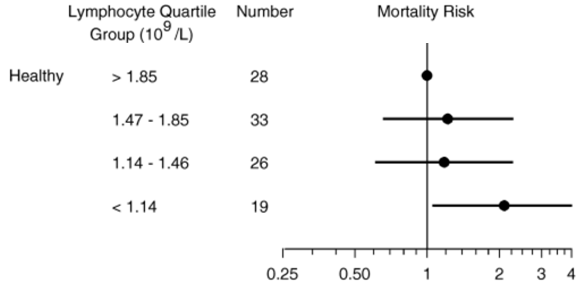
In a small study of 106 older adults (> 85y) that were healthy (i.e. free of disease) at baseline, lymphocytes less than 1.14*10^9 cells/L (equivalent to 1140*10^6 cells/L) was associated with an increased risk of death for all causes, when compared with 1850*10^6 cells/L (Izaks et al. 2003):
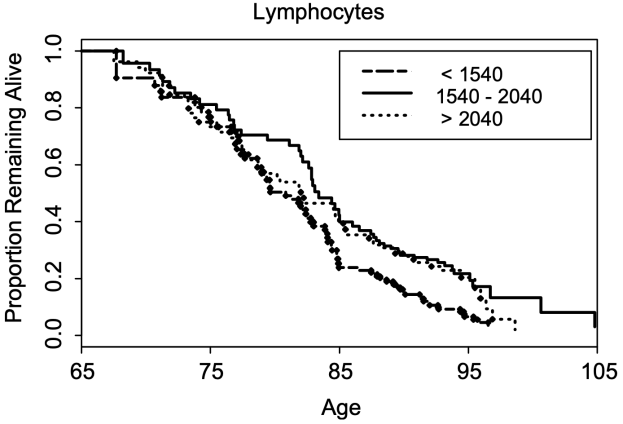
In a larger study (624 subjects), lymphocytes less than 1540*10^6 cells/L was associated with a significantly shorter average lifespan (~5y; 0.5 proportion remaining below), when compared with 1540 – 2040*10^6 cells/L . Also note that survival for the group that had 1540 – 2040*10^9 lymphocytes/L was not significantly different from the group that had more than 2040*10^9 lymphocytes/L (Leng et al. 2005):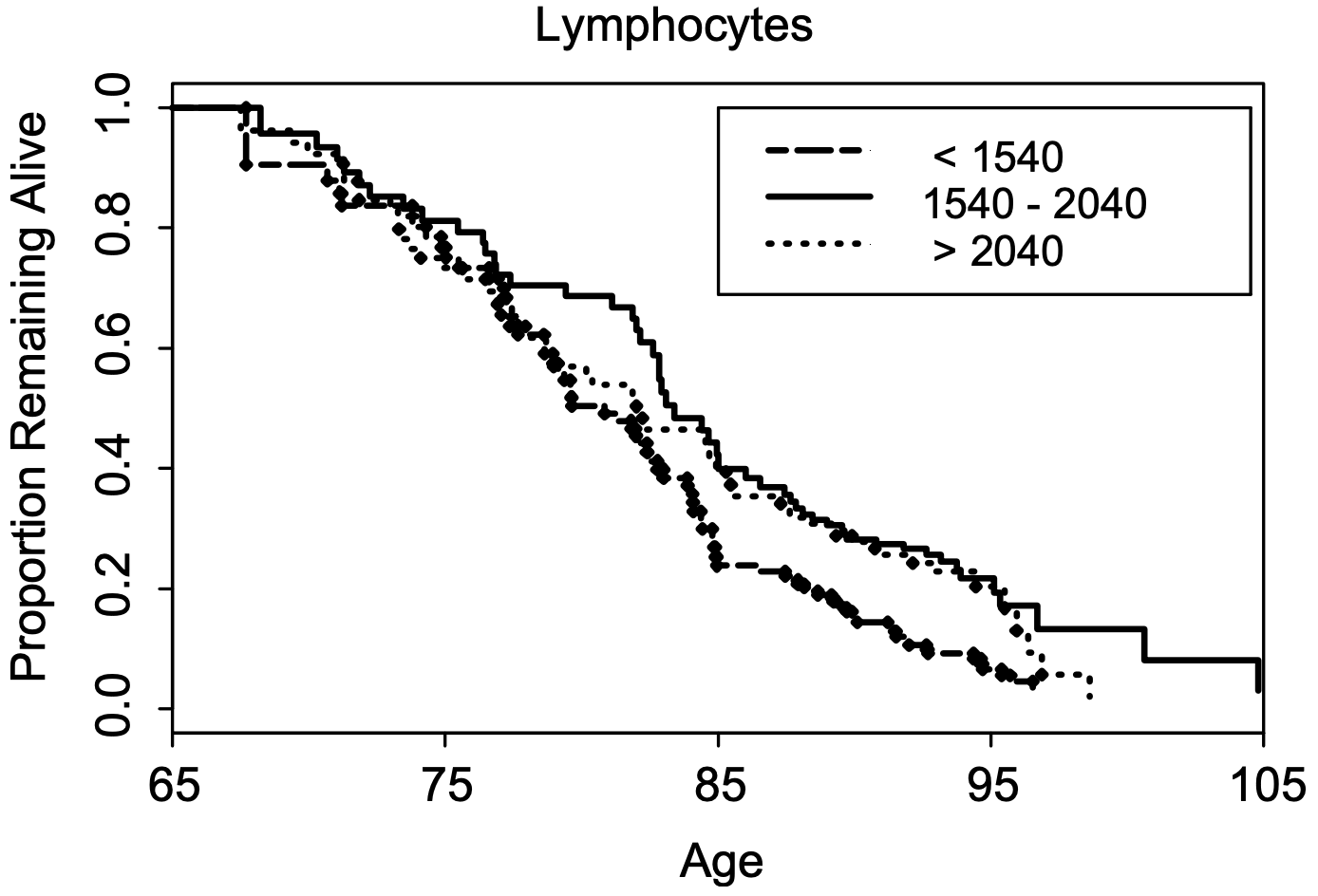
In agreement with the smaller studies, lymphocytes < 1300 and < 1200*10^6 cells/L in women and men (red and blue, far left), respectively was associated with an increased all-cause mortality risk, when compared with average lymphocyte values ~1900*10^6 cells/L (decile 5) in a larger study that included 262,394 non-smokers (age range, 37 – 73y; Welsh et al. 2018):
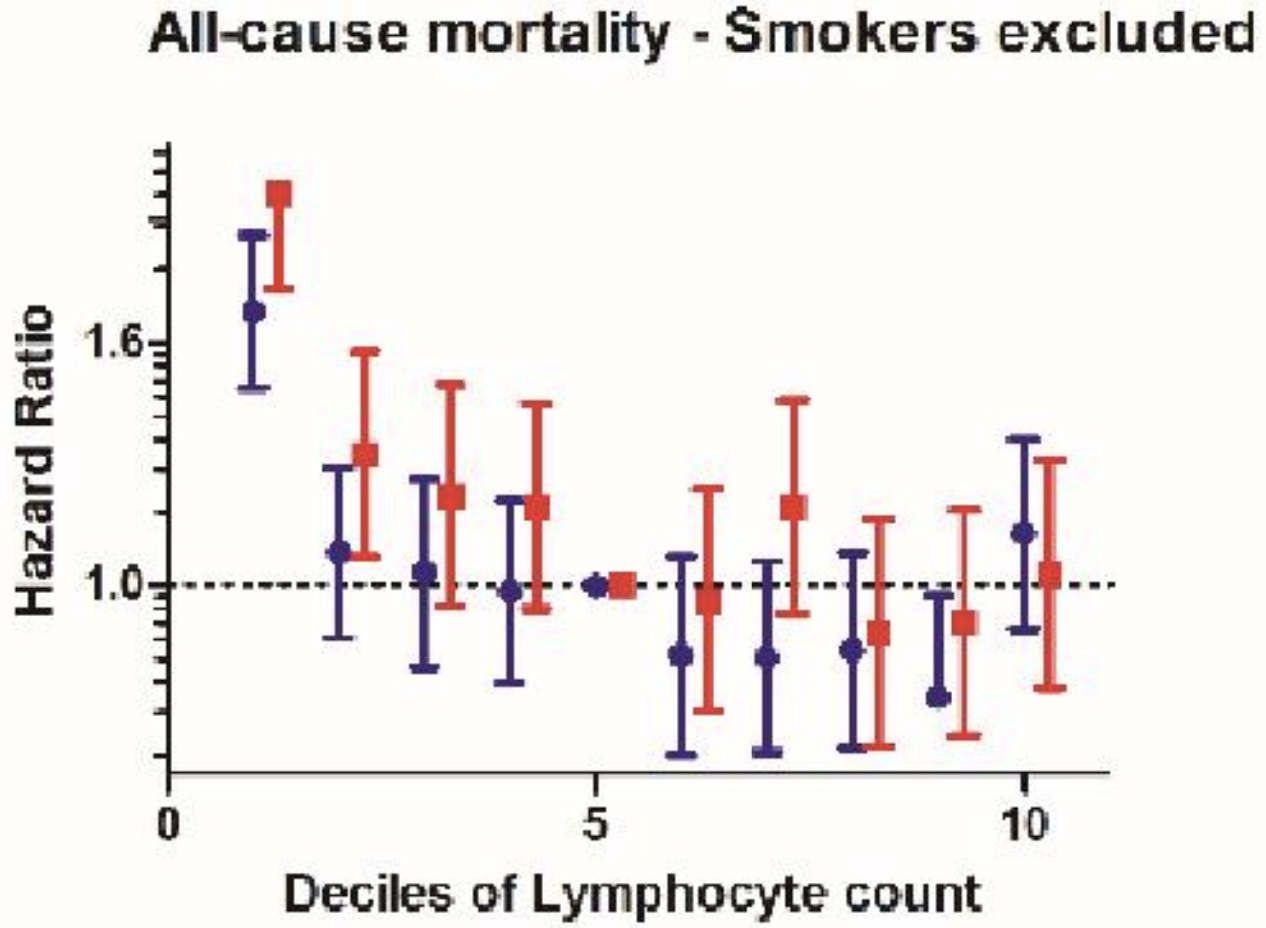
Collectively, these data suggest that higher values for lymphocyte % and for the absolute amount of lymphocytes may be optimal for minimizing disease risk and for maximizing longevity. If both are low, can they be raised? Circulating levels of lymphocytes are reduced during zinc deficiency (Fraker and King, 2001), so monitoring zinc intake, then increasing it to at least the RDA may be a first step towards increasing lymphocyte levels and %.
If you’re interested, please have a look at my book!
References
Fraker PJ, King LE. A distinct role for apoptosis in the changes in lymphopoiesis and myelopoiesis created by deficiencies in zinc. FASEB J. 2001 Dec;15(14):2572-8.
Izaks GJ, Remarque EJ, Becker SV, Westendorp RG. Lymphocyte count and mortality risk in older persons. The Leiden 85-Plus Study. J Am Geriatr Soc. 2003 Oct;51(10):1461-5.
Leng SX, Xue QL, Huang Y, Ferrucci L, Fried LP, Walston JD. Baseline total and specific differential white blood cell counts and 5-year all-cause mortality in community-dwelling older women. Exp Gerontol. 2005 Dec;40(12):982-7.
Levine ME. Modeling the rate of senescence: can estimated biological age predict mortality more accurately than chronological age? J Gerontol A Biol Sci Med Sci. 2013 Jun;68(6):667-74. doi: 10.1093/gerona/gls233.
Wang Z, Li L, Glicksberg BS, Israel A, Dudley JT, Ma’ayan A. Predicting age by mining electronic medical records with deep learning characterizes differences between chronological and physiological age. J Biomed Inform. 2017 Dec;76:59-68. doi: 10.1016/j.jbi.2017.11.003.
Welsh C, Welsh P, Mark PB, Celis-Morales CA, Lewsey J, Gray SR, Lyall DM, Iliodromiti S, Gill JMR, Pell J, Jhund PS, Sattar N. Association of Total and Differential Leukocyte Counts With Cardiovascular Disease and Mortality in the UK Biobank. Arterioscler Thromb Vasc Biol. 2018 Jun;38(6):1415-1423. doi: 10.1161/ATVBAHA.118.310945.